The focus has come back to finding non-invasive ways to reduce body weight, says S.Ananthanarayanan.
With diets and exercise proving only mildly effective in weight reduction, there is more and more reliance being placed on surgical methods to reduce food intake and metabolism, to save the obese from a host of troubles that arise from overweight. But surgery, although undoubtedly effective, is often not ‘palatable’ and also has its own problems. A discovery that surgery depends on other factors to have results has renewed the quest for methods to control weight gain without the need for surgery.
Karen K. Ryan, Valentina Tremaroli, Christoffer Clemmensen, Petia Kovatcheva-Datchary, Andriy Myronovych, Rebekah Karns, Hilary E. Wilson-Perez, Darleen A. Sandoval, Rohit Kohli, Fredrik Backhed and Randy J. Seeley, of Ohio, Cincinati, Gotherburg in Sweden, and Copenhagen report in the journal, Nature, their finding that surgery, which seems to mechanically impede over-eating or assimilation of food, still does not prove effective if a genetic feature is not present.
Obesity is classified as a disease and is considered the one main preventable cause of death in current times. Overweight is directly implicated in heart disease, type 2 diabetes, a disease of breathing obstruction during sleep, some kinds of cancer, degeneration of the bones and asthma. Records show that the overload of body weight is a major cause for the need of knee and hip replacements. And there are conditions where reduction of body weight is an imperative for survival.
While active living style and moderation in consumption of food are certainly the best way to weight control, the reason for overweight may be genetic, medical or psychiatric. The increased availability and use of attractive, high calorie ‘fast food’, use of private and public transport and mechanization of much that was done manually are causes that have increased in modern times. Other reasons for the increase in obesity are identified or suspected as lack of sleep, hormonal imbalance due to pollution or contaminants or some medicines, stable ambient temperature, thanks to air conditioning, and the rise of genetically overweight populations due to economic or social reasons. But the bottom-line is that obesity, or unreasonable weight gain, is a disease with serious implications and there are situations where it is vital that it be reversed.
Bariatric surgery
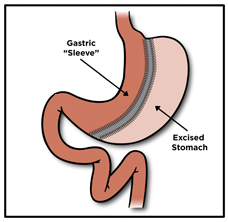
Where there are reasons that a person is not able to reduce food intake or increase exercise, or the over-weight is due to other reasons, the solution that is available and sometimes unavoidable is surgery. By surgery we mean not the ‘liposuction’, which is cosmetic, but of the stomach and digestive system, to restrict the amount of food that can be taken or to interfere with assimilation. Methods include reducing the size of the stomach with a band, or removing a part of the stomach or bypass of a portion of the small intestines. A common procedure used is the Vertical Sleeve Gastrectomy, where 80% of the stomach is removed by surgically reshaping the bulge shape into a sleeve that matches the food pipe and the beginning of the small intestine. The procedure is carried out laproscopically and is becoming widespread and carried out even on children and adolescents. The procedure has been found to be so successful in weight control that it has replaced other methods, like bypass of a part of the intestine. The method has been found to clearly effective and also superior to other, medical methods of managing over-weight or diseases that arise for obesity.
Surgical methods are found to be effective almost every time and the results are sustained and long term. There is marked improvement in all associated medical conditions and diabetes is found to be fully controlled within a year in 40% of the cases.
While VSG has thus become the way to go for the overweight, there are negatives that do not make surgery an easy choice for all patients. For one, the procedure is non-reversible. The reduction in food intakes is because the patient feels nausea as soon as the restricted stomach is full and she stops eating to avoid discomfort, rather than out of satiation. And then, there are the risks of surgery and complications, such as ‘sleeve leaks’, clots and infection, damage to the Vagus nerve, which causes constant nausea, vomiting and disturbance in the normal passage of food. There is hence the need for alternative, non-surgical methods. But the great effectiveness and wide use of VSG has led to a feeling that it is the only ‘way to go’.
On the face of it, it would appear that the results of VSG come from reduction in food intake because of a physically smaller stomach – a form of mechanical intervention. And the simplicity of this explanation suggests that there is nothing more to be said – the root of the trouble is in filling the stomach and if the stomach is made smaller, it settles the matter. But there is evidence that only reduction of size may not be the mechanism leading to disease remission. For one, it is found that most diabetic patients are able to go off diabetes medication within days of surgery. But in this short time there is hardly any substantial weight reduction. How then to explain the dramatic relief? There is hence doubt about mechanical reduction being the reason for VSG results and it would appear that VSG affects other processes. It has been suggested that the results arise from changes in gut physiology, changes in nerve mediated signaling or the nature of microbes that populate the intestines.
A well known result of weight reduction surgery is that there are changes in the circulation of bile acids, the secretions of the liver, which are used in the assimilation of fats. It has also been established that in addition to the mechanical digestion and absorption of fats, bile acids combine with a factor known as FXR, which plays a role in the metabolism of fats. In the light of this effect of VSG, the group of researchers examined the role that the FXR link may have in regulating metabolism and the microbial environment of the gut.
Testing the link
To test out this possibility, the researchers carried out VSG surgery on groups of mice that were obese by being overfed. One group of mice had been genetically modified to lack the FXR factor and the other group was of unmodified mice from the same litter. They used methods of analysis of the behavior of cells to trace the biological processes that got changed after VSG. The group had earlier established that VSG had a major effect the way genes of the liver acted in regulating fats. They now found that the biological pathway that led to metabolism and conversion of fats was the key beneficiary of VSG. Of other pathways strongly benefitted, several were found to point to changes in microbe populations.
The trials clearly established that it was only the mice which had the FXR process intact that benefited from VSG. There was weight loss and appetite restriction of the modified group too, but this was not sustained and this group soon lost the apparent benefit. Even in respect of the changes in the microbe populations in the gut, which affected weight gain and glucose control, it was found that VSG had significantly greater effect on mice that had the FXR factor than ones that did not.
These are significant findings, as they point to mechanisms of weight control through VSG that are quite different from pure dimensional reduction of the stomach volume. As an FXR linked mechanism is demonstrated, it suggests that there could be other means of reaching the desired end, without the need for surgery.
' ------------------------------------------------------------------------------------------